Recently one of my family members who is a ‘young’ older adult, think of a 70-year-old who looks 55 and does cardio-kickboxing (yes, I’m jealous, too), said to me “I messed up on my meds.” They went on to share that they had mistaken one med for another when the pharmacy changed generic suppliers of a longstanding medication they had been on and the new formulation made the tablet look nearly identical to another medication they take. This led to them inadvertently taking two tablets of a medication that they should have only taken one. Being very tuned in to their body, the individual noted a few hours later that they “just weren’t feeling right.” This prompted them to think about what could be contributing to their symptoms and medications due to the recent trip to the pharmacy. Their quick awareness of the potential that the symptoms could be and in fact were medication related prevented further complications; they were able to identify what had happened, adjust their approach accordingly and advert a catastrophe. The consequences of not identifying these symptoms as medication related could have been fatal.
Every year thousands of older adults die of potentially preventable medication related causes. The CDC notes that 1.3 million ER visits annually are due to adverse drug events. About 350,000 individuals require hospitalization for further treatment due to medications. Older adults tend to take more medications than younger individuals and are at risk for the consequences of polypharmacy – the use of multiple medications often prescribed by multiple healthcare providers combined many times with use of over-the-counter medications – that can create a recipe for disaster including falls, confusion, hospitalization and even institutionalization if not detected and corrected.
So how to avoid a medication “mess up?” Here are some tips/approaches to consider:
KNOW YOUR MEDICATIONS
There are a number of things you should know about your medications: What do they look like, what are they for, what is the amount (number of tablets and dose) that you should be taking, when are you to take them, when are you to stop taking them, what are the side effects, what are the additional instructions you need to be aware of, when does the prescriber want to be notified?
Keep a list of your current medications including over the counter medications you are using – bring the list with you when you go to the pharmacy or to a healthcare appointment.
ASK QUESTIONS
When you are not sure of the answers to any of the above, ask questions: Ask your prescriber, ask the pharmacist, ask a friend or family member who may be better able to navigate some of the complexities of your medication regimen. It can be helpful to make a list to bring with you for your next pharmacy visit or health appointment.
BE WARY OF ADDING MORE
When a new medication is started, be sure to ask if there are any current medications that could be discontinued. I believe in taking a “less is more approach” with medications in the elderly and while that may not always be possible, it doesn’t hurt to ask. Be mindful also of what you are adding by use of over the counter/non-prescribed medications including herbals and nutraceuticals. Just because you don’t need a prescription doesn’t mean these medications are without concern. They may interact with your prescribed medications. It’s best to check with a pharmacist or the prescriber.
DON’T TAKE EXPIRED MEDICATIONS
Medications expire. Be mindful of the age of a prescription and if it is a medication only taken as needed, just because there are pills left over, they may no longer be safe to take. Check the labels on over the counter and prescribed medications.
DON’T SHARE MEDICATIONS
Prescribers take time to select medications that work best for you as an individual in consideration of your age, your weight, your health condition, and other variables. What works for you may not work the same for others and may cause a problem rather than help with a problem.
USE HELPFUL TOOLS
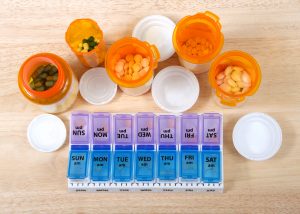
There are many medication tools available including pill boxes, pill dispensers with alarms, apps on your electronic devices and phones, wearable devices that can send reminders and provide information about your medications.
CONSIDER OUTSIDE HELP
When your medication regimen becomes too complex for you to manage and your health is suffering the consequences and friends and family are unable to assist, it is wise to consider using outside help to ensure that your medications are taken safely. Many home care providers offer this service – be sure to check with your healthcare provider for recommendations. Unfortunately, medication assistance service at home is generally not covered by Medicare or most private insurance and has to be paid for out-of-pocket. Still a worthwhile expense if it reduces the likelihood of a negative event
Knowledge is power – now you know – a medication mess up can have dire consequences but the potential for a bad outcome can be reduced – don’t let it happen to you!
Main Image Credit – © 2019 BrightStar Care®


